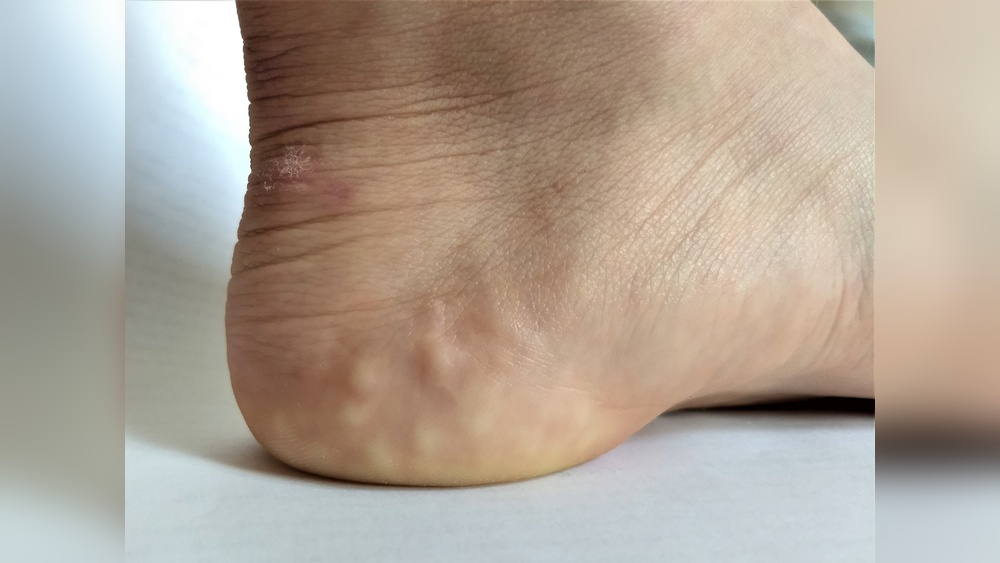
Have you ever noticed small, soft bumps appearing on your heels or wrists when you put pressure on them? These tiny lumps might be piezogenic papules—a common but often misunderstood skin condition.
You might wonder if they are painful or if they mean something serious for your health. Understanding what piezogenic papules are, why they appear, and how they affect you can help ease your concerns and guide you to the right care.
Keep reading to discover everything you need to know about piezogenic papules and how to manage them effectively.
Causes Of Piezogenic Papules
Piezogenic papules are small, soft bumps that appear on the heels or wrists. These bumps occur due to fat pushing through the connective tissue under the skin. Understanding the causes of piezogenic papules helps in recognizing why they develop and who might be more prone to them. Several factors contribute to their formation, including pressure on the skin, genetic predisposition, and certain medical conditions. This section explores these causes in detail.
Role Of Pressure On The Skin
Pressure plays a crucial role in the appearance of piezogenic papules. These bumps usually form in areas that experience frequent or intense pressure. For example, the heels carry the body’s weight during standing and walking, making them common sites for these papules.
Repeated pressure causes fat from the deeper layers to push through weak spots in the skin’s connective tissue. This protrusion creates visible small lumps.
- Standing or walking for long periods increases pressure on the heels.
- Wearing tight shoes can add more pressure to certain foot areas.
- Activities like running or jumping raise the stress on skin and fat layers.
The following table shows common activities linked to higher pressure and piezogenic papules risk:
| Activity | Effect on Skin Pressure | Risk Level |
|---|---|---|
| Standing for hours | Constant pressure on heels | High |
| Running | Repeated impact on feet | Medium |
| Wearing tight footwear | Localized pressure points | Medium |
| Sitting or resting | Minimal pressure | Low |
Pressure weakens the connective tissue over time, allowing fat to bulge out. Those who stand or move a lot have a higher chance of developing piezogenic papules.
Genetic Factors
Genetics can influence who develops piezogenic papules. Some people inherit weaker connective tissue, making it easier for fat to push through.
Family history often plays a role. If parents or siblings have piezogenic papules, others in the family might get them too.
Key genetic aspects include:
- Inherited connective tissue weakness: This reduces skin strength and elasticity.
- Collagen production defects: Collagen is important for skin support and repair.
- Skin structure differences: Some people naturally have thinner or more fragile skin layers.
Studies suggest genetic disorders affecting connective tissue can increase the chance of piezogenic papules. These conditions often show symptoms like stretchy skin, joint hypermobility, or easy bruising.
Genetic influence does not guarantee papules but raises the risk. The combination of genetics and pressure usually leads to the bumps appearing.
Associated Medical Conditions
Certain medical conditions link to piezogenic papules because they weaken skin or connective tissue. These conditions make it easier for fat to protrude.
Common associated conditions include:
- Ehlers-Danlos Syndrome (EDS): A disorder causing very stretchy, fragile skin and loose joints.
- Obesity: Extra body weight adds pressure on the feet and skin.
- Flat feet (pes planus): Change foot structure and increase stress on heels.
- Connective tissue diseases: Conditions like Marfan syndrome that affect skin and ligaments.
People with these conditions have:
- Weaker skin support.
- Higher skin elasticity.
- More pressure on fat layers.
These factors combine to cause piezogenic papules more easily than in healthy individuals.
Understanding these links can help doctors identify underlying issues and offer better advice for managing or preventing papules.
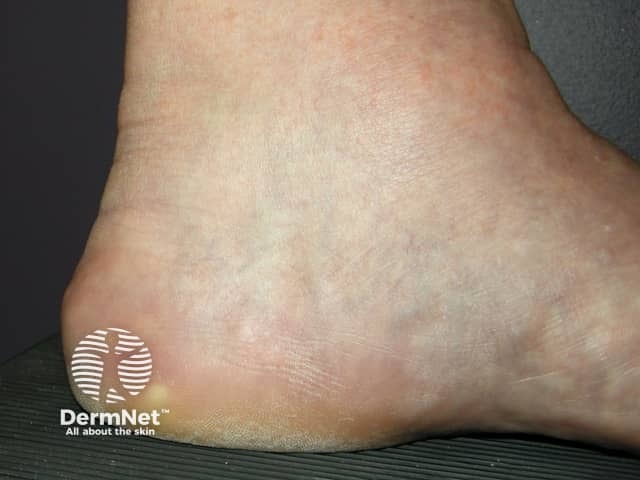
Credit: dermnetnz.org
Symptoms And Appearance
Piezogenic papules are small, benign skin lesions that appear on the feet. These pressure-induced papules form due to subcutaneous fat herniation through connective tissue. They often occur in weight-bearing areas of the foot, causing concern for many. Understanding the symptoms and appearance of these papules helps in identifying them early and knowing when to seek Piezogenic papules treatment.
Typical Locations
Foot papules usually develop in specific areas where pressure is highest. These locations are prone to repeated stress from standing, walking, or running. The most common sites include:
- Heel papules: Found around the heel, these are the most frequent spots for Piezogenic papules.
- Side edges of the feet: Papules can appear along the outer edges where the foot bears weight.
- Pressure points: Areas exposed to constant friction or pressure during activities.
These locations are critical because they are weight-bearing areas where connective tissue may weaken. The subcutaneous fat beneath the skin pushes through small gaps, causing visible papules. People with connective tissue disorder may notice more frequent or severe foot papules. Identifying typical locations helps distinguish Piezogenic papules from other skin conditions.
| Location | Description | Commonality |
|---|---|---|
| Heel | Back part of the foot, main weight-bearing area | Very common |
| Foot sides | Outer edges near the arch and toes | Common |
| Pressure points | Areas exposed to repeated friction | Less common |
Visual Characteristics
Piezogenic papules show distinct visual signs that help in diagnosis. They appear as small, soft bumps on the skin’s surface. Their size and shape can change based on pressure and foot position.
- Typically, papules are round or oval.
- Color ranges from skin-toned to slightly yellowish.
- They become more noticeable when standing or bearing weight.
- When the foot is lifted, papules often flatten or disappear.
These papules result from fat herniation through weakened connective tissue. The skin may stretch slightly, revealing the underlying subcutaneous fat pushing outward. Unlike other lesions, Piezogenic papules do not show redness or inflammation unless irritated. They are benign skin lesions, meaning they are not harmful but can cause concern due to their appearance.
Visual signs to watch for:
- Multiple small bumps on the heel or foot edges
- Soft texture when pressed
- Changes with pressure or foot position
Pain And Discomfort Levels
Not all Piezogenic papules cause pain. Many people notice these papules without discomfort. Pain or foot pain appears in some cases, especially after prolonged standing or walking.
Pain levels vary and may include:
- Mild discomfort: Slight aching during pressure on the foot.
- Sharp pain: Occurs if the papules become irritated or inflamed.
- No pain: Many have painless papules that only affect appearance.
The pain happens because the herniated fat can press on nerves or surrounding tissues. Individuals with connective tissue disorder often report more discomfort. Pain may improve with rest or by reducing pressure on the feet. Proper Piezogenic papules treatment focuses on relieving foot pain and avoiding activities that worsen symptoms.
| Symptom | Description | Frequency |
|---|---|---|
| No pain | Visible papules without discomfort | Most cases |
| Mild pain | Aching or tenderness on pressure | Some cases |
| Severe pain | Sharp pain due to irritation | Few cases |
Diagnosis Methods
Piezogenic papules are small, soft bumps that appear on the heels or feet. These papules occur due to fat pushing through the connective tissue under the skin. Proper diagnosis is essential to distinguish piezogenic papules from other foot conditions. Several methods help doctors confirm the diagnosis and decide on treatment options.
Physical Examination
The first step in diagnosing piezogenic papules is a thorough physical examination. Doctors carefully inspect the feet and heels, especially when the patient stands or applies pressure. Piezogenic papules become visible as small, soft lumps on the heels under weight-bearing conditions.
Key points during physical examination include:
- Observation of soft, skin-colored bumps on the heel.
- Checking if the papules disappear when pressure is relieved.
- Assessing for pain or tenderness at the site of the bumps.
- Asking about the history of foot pain or trauma.
Doctors may ask the patient to stand on tiptoes or press the heel to see how the papules respond. This helps confirm that the lumps are caused by fat herniation. Physical examination is usually enough to diagnose piezogenic papules because of their typical appearance and behavior.
| Examination Step | Purpose | What to Look For |
|---|---|---|
| Visual Inspection | Identify visible papules | Soft, skin-colored bumps on heels |
| Weight Bearing Test | Observe papules under pressure | Bumps become prominent when standing |
| Palpation | Check tenderness or pain | Pain at papule sites or soft texture |
Imaging Techniques
Imaging helps confirm the diagnosis and rule out other conditions. Ultrasound is the preferred method for visualizing piezogenic papules. It shows the fat lobules pushing through connective tissue clearly.
Benefits of ultrasound include:
- Non-invasive and painless procedure.
- Real-time images of soft tissue layers.
- Ability to detect fat herniation and tissue changes.
In some cases, magnetic resonance imaging (MRI) may be used. MRI offers detailed views of soft tissues and can help if the diagnosis is uncertain. X-rays are less useful but may be done to exclude bone problems.
Comparison of imaging techniques:
| Imaging Type | Use | Pros | Cons |
|---|---|---|---|
| Ultrasound | Detect fat herniation | Quick, safe, cost-effective | Operator-dependent accuracy |
| MRI | Detailed soft tissue imaging | High-resolution images | Expensive, less accessible |
| X-ray | Exclude bone issues | Widespread availability | Not useful for soft tissue |
Differential Diagnosis
Doctors must distinguish piezogenic papules from other similar foot conditions. Several disorders may mimic piezogenic papules but require different treatments.
Common conditions to consider include:
- Plantar fibromatosis: Firm nodules in the foot’s arch, not soft papules.
- Ganglion cysts: Fluid-filled lumps usually near joints or tendons.
- Heel pads atrophy: Thinning of fat pads causing pain, without lumps.
- Fat herniation due to trauma: Similar lumps but following injury.
Doctors review symptoms, physical exam, and imaging to rule out these conditions. For example, ganglion cysts feel firmer and do not change with pressure. Plantar fibromatosis nodules are fixed and usually in a different location.
Summary table for differential diagnosis:
| Condition | Key Features | Differences from Piezogenic Papules |
|---|---|---|
| Plantar Fibromatosis | Firm nodules on foot arch | Firm, fixed lumps; not pressure-dependent |
| Ganglion Cysts | Fluid-filled lumps near joints | Firm, no change with pressure |
| Heel Pad Atrophy | Pain without lumps | No visible papules; thinning fat pad |
| Traumatic Fat Herniation | Lumps after injury | History of trauma; may be tender |
Treatment Options
Piezogenic papules are small, soft bumps that appear on the heels due to fat herniation through the connective tissue. Many people experience no pain, but some find them uncomfortable or painful, especially after standing or walking for long periods. Various treatment options exist, ranging from simple lifestyle changes to medical and surgical methods. Choosing the right treatment depends on the severity of symptoms and personal needs.
Conservative Management
Conservative management is often the first step for treating piezogenic papules. This approach focuses on reducing pressure on the heels and easing discomfort without invasive procedures.
- Footwear modification: Wearing shoes with thick, cushioned soles helps absorb impact and reduce pain.
- Orthotic inserts: Custom or over-the-counter heel pads provide extra support and cushion.
- Activity adjustment: Limiting prolonged standing or walking can prevent worsening symptoms.
- Weight management: Maintaining a healthy weight lowers pressure on the feet.
- Compression stockings: These can help support the feet and reduce swelling.
These methods are safe and simple. Most people find relief by combining several conservative strategies. It may take a few weeks to notice improvements. Regular foot care and avoiding hard surfaces also help.
Medical Interventions
Medical interventions target pain relief and reduce the appearance of piezogenic papules when conservative measures fall short. These treatments require professional guidance from a healthcare provider.
- Corticosteroid injections: These reduce inflammation and pain around the papules.
- Local anesthetics: Temporary pain relief can be achieved through local numbing injections.
- Sclerotherapy: Injection of a sclerosing agent helps shrink the fat herniation.
- Physical therapy: Specialized foot exercises improve muscle strength and foot support.
| Treatment | Purpose | Effect Duration |
|---|---|---|
| Corticosteroid Injections | Reduce inflammation and pain | Several weeks |
| Sclerotherapy | Shrinks fat herniation | Several months |
| Physical Therapy | Strengthens foot muscles | Ongoing |
Medical treatments often complement conservative care. They are suitable for those with persistent pain. Discuss risks and benefits with a doctor before proceeding.
Surgical Approaches
Surgery is the last option for severe or painful piezogenic papules. It involves repairing or removing the fat herniation to relieve symptoms.
- Fat excision: Removal of herniated fat through small incisions.
- Fascial repair: Strengthening or tightening the connective tissue to prevent fat protrusion.
- Liposuction: Suctioning out excess fat to reduce papules.
These procedures require anesthesia and have recovery times ranging from days to weeks. Risks include infection, scarring, and possible recurrence of papules.
Surgical treatment suits people with intense pain or cosmetic concerns. Choosing surgery should involve a detailed discussion with a foot specialist. Post-surgery care includes rest, wearing protective footwear, and follow-up visits.
Prevention And Lifestyle Tips
Piezogenic papules are small, soft bumps that appear on the heels. They happen when fat pushes through the skin due to pressure or strain. These papules can be painful or annoying. Prevention and lifestyle changes help reduce discomfort and lower the chance of getting more papules. Simple steps make a big difference in managing this condition.
Footwear Recommendations
Choosing the right shoes plays a crucial role in preventing piezogenic papules. Shoes should provide good cushioning to reduce pressure on the heels. Avoid hard soles or shoes with thin padding. Look for footwear with a thick, soft sole that absorbs shock well.
Here are some tips for picking proper shoes:
- Use shoes with arch support to distribute weight evenly.
- Pick shoes with a wide heel area to avoid squeezing the foot.
- Choose shock-absorbing insoles for extra comfort.
- Replace worn-out shoes often to maintain support.
- Avoid high heels and flat shoes without padding.
| Footwear Type | Recommended | Not Recommended |
|---|---|---|
| Running shoes | Yes, with good cushioning | No, if soles are worn out |
| High heels | No | Yes, increase heel pressure |
| Flip-flops | No | Yes, lack support |
| Orthopedic shoes | Yes, if fitted properly | No, if tight or hard |
Activity Modifications
Activities that put pressure on heels can cause or worsen piezogenic papules. Adjusting daily movements helps protect the feet. Try to reduce time spent standing or walking on hard surfaces. Use soft mats or cushioned flooring at work or home.
Follow these activity tips:
- Limit standing for long periods; take breaks often.
- Avoid running or jumping on hard ground.
- Use padded insoles during exercise or sports.
- Switch to low-impact exercises like swimming or cycling.
- Stretch calf muscles regularly to reduce foot strain.
These changes reduce pressure on the heel fat, preventing papules from forming or getting worse. Listen to your body and rest if the heel feels sore or tender.
Skin Care Practices
Good skin care keeps the heel healthy and less prone to piezogenic papules. Moisturized skin is more elastic and better at handling pressure. Dry, cracked skin can increase discomfort and risk of injury.
Use these skin care steps:
- Wash feet daily with mild soap and warm water.
- Apply a thick moisturizer or heel balm after washing.
- Use products with ingredients like urea or glycerin for deep hydration.
- Gently exfoliate rough skin to remove dead cells once a week.
- Wear clean socks made of breathable materials like cotton.
Keeping feet clean and soft lowers irritation and helps the skin handle pressure better. Avoid harsh soaps or hot water, which dry out the skin. Regular care supports overall foot health and comfort.

Credit: www.dermatologyadvisor.com
When To Seek Medical Advice
Piezogenic papules are small, benign skin lesions that appear on the heel or side of the foot. These pressure-induced papules happen due to fat herniation through connective tissue in the foot. Most people notice them when standing or putting weight on their feet. Usually, piezogenic pedal papules cause no pain or serious problems. Knowing when to seek medical advice is important, especially if symptoms change or worsen. Early foot pain diagnosis helps manage any discomfort and rule out other issues.
Warning Signs
Most piezogenic papules are harmless and painless. Warning signs mean that something more serious may be happening. Pay attention to these signals:
- Sudden increase in size or number of the nodules on your heels
- Severe pain that does not go away with rest
- Redness, swelling, or warmth around the papules
- Ulceration or bleeding from the affected skin
- Changes in skin color near the papules
These warning signs can indicate infection, inflammation, or other connective tissue disorder complications. They need prompt medical attention to avoid worsening conditions. A doctor can perform a thorough foot pain diagnosis and suggest the right piezogenic papules treatment.
Persistent Symptoms
Sometimes, piezogenic papules symptoms last longer than expected. Persistent pain or discomfort requires a medical checkup. Typical symptoms to monitor:
- Ongoing heel pain nodules that hurt during standing or walking
- Fat herniation foot feeling tender or sensitive to touch
- Difficulty wearing shoes due to pressure-induced papules
- Pain that worsens with activity but does not improve with rest
Long-term symptoms may affect daily activities and quality of life. Doctors may recommend imaging tests or physical exams to confirm the diagnosis. Persistent symptoms suggest the need for customized piezogenic papules treatment options. Ignoring these signs can lead to increased discomfort and complications.
Complications To Watch For
Piezogenic papules rarely cause serious complications. Still, some cases develop problems that require medical care. Complications include:
| Complication | Description | Possible Result |
|---|---|---|
| Infection | Breaks in the skin can allow bacteria in | Redness, swelling, and increased pain |
| Chronic pain | Repeated pressure leads to long-lasting discomfort | Difficulty walking and reduced mobility |
| Connective tissue disorder | Underlying issues weaken the foot’s structure | More fat herniation and worsening papules |
Watch for signs of complications such as fever, spreading redness, or worsening pain. These signs require immediate consultation with a healthcare provider. Early treatment prevents long-term damage and helps manage the condition effectively.

Credit: www.jpeds.com
Frequently Asked Questions
What Causes Piezogenic Papules On Feet?
Piezogenic Papules are caused by fat herniation through the heel’s connective tissue. Pressure from standing or walking triggers their appearance. They often occur in athletes or people who stand for long periods. The condition is harmless but can cause discomfort.
Are Piezogenic Papules Painful Or Dangerous?
Piezogenic Papules are usually painless and harmless. However, some people experience mild pain or discomfort when standing. The papules disappear when pressure is relieved. They do not cause serious health issues or require aggressive treatment.
How Can Piezogenic Papules Be Treated Effectively?
Treatment includes reducing pressure on the heel, using cushioned insoles, and avoiding prolonged standing. In painful cases, compression bandages or orthotics help. Rarely, surgical options are considered. Most people manage symptoms with simple lifestyle adjustments.
Can Piezogenic Papules Disappear On Their Own?
Yes, Piezogenic Papules often disappear when pressure is removed. They are temporary and usually fade when sitting or resting. Consistent pressure causes them to reappear. Managing activity levels and footwear helps reduce their visibility.
Conclusion
Piezogenic papules are small, harmless bumps on the skin. They often appear when pressure is on the feet or hands. Most people do not need treatment for them. Wearing comfortable shoes can help reduce discomfort. Seeing a doctor is good if pain or changes occur.
Understanding these papules helps ease worry and manage symptoms. Simple care often keeps them from bothering daily life. Keep an eye on any changes and stay informed.